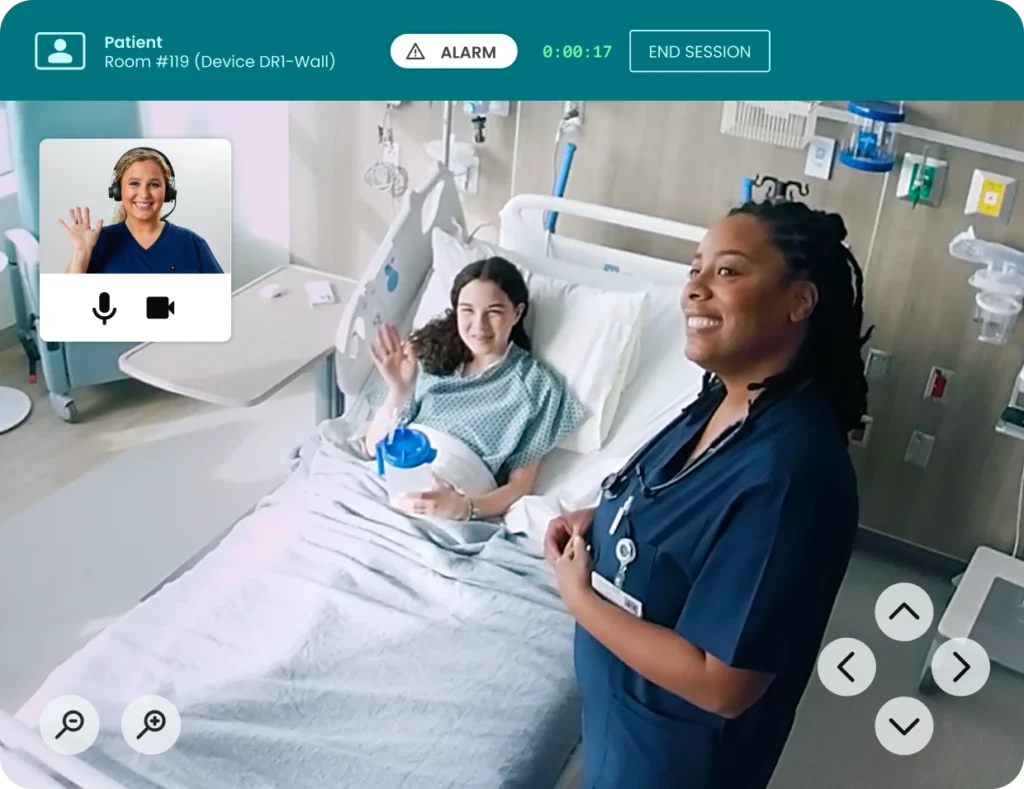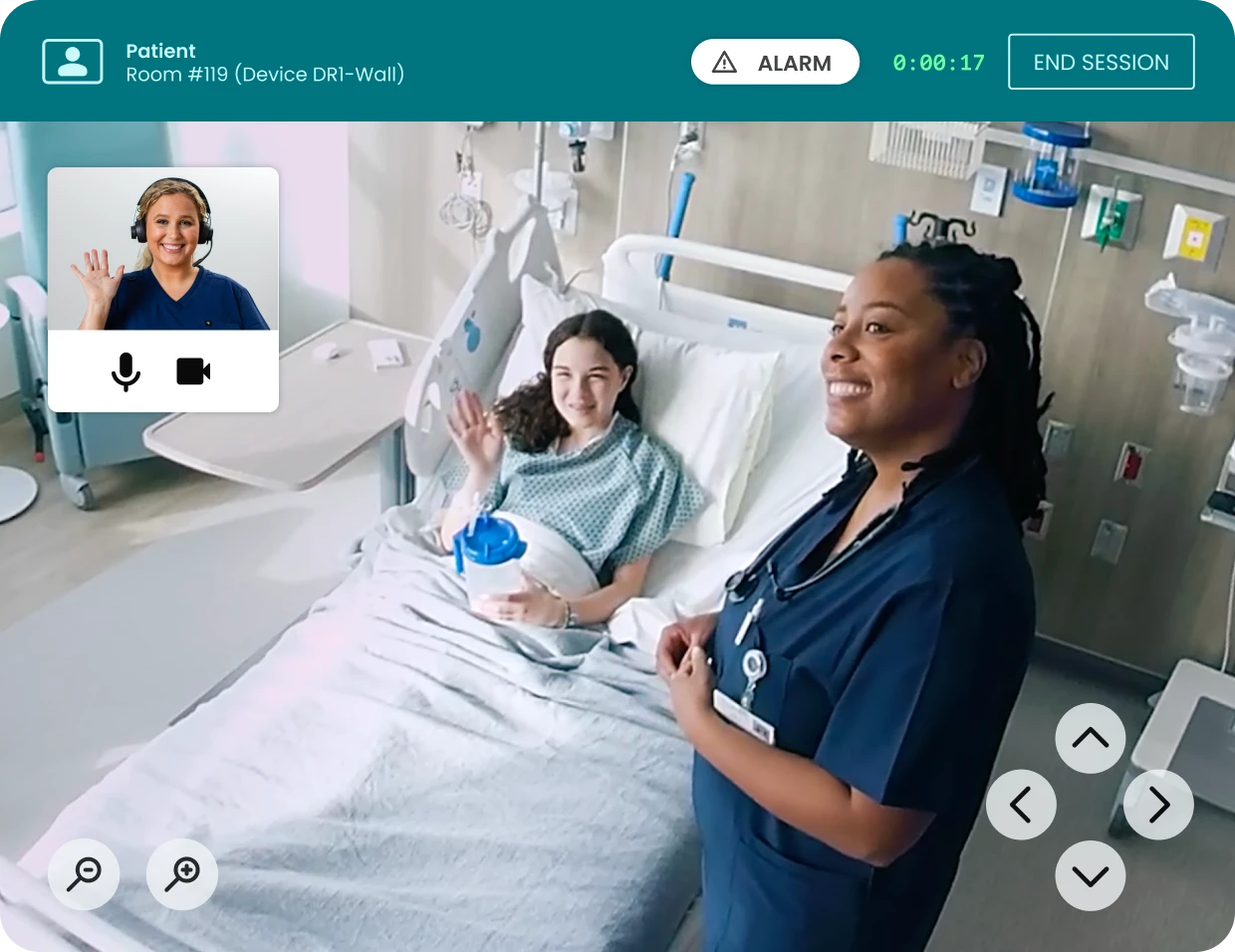
More than half of U.S. nurses report burnout and ongoing mental health challenges — impacting both caregiver wellbeing and patient outcomes.
National Nurses Week and Mental Health Awareness Month share the same calendar for good reason. The people we trust most with our lives are facing a crisis of their own. More than half of U.S. nurses report burnout and mental health challenges, impacting both caregiver wellbeing and patient outcomes. Burnout affects up to 56% of the nursing workforce, driven by high stress, chronic understaffing, and administrative burden. In recent years, there has been an influx of nurse walkouts and strikes. In January 2026, roughly 15,000 nurses in New York walked off the job in what became the largest nurse strike in the state’s history—a breaking point fueled by dangerous understaffing, rising workplace violence, and unsustainable workloads.” This moment presents an important opportunity to better support nurses and strengthen the care they provide every day.
When nurses are overwhelmed, everyone feels it. Patient safety suffers. Staff turnover climbs. And the cycle only deepens. Our nurses give 12+ hours a day to caring for others — but who is caring for them? They are some of the most resilient people in any room, but resilience has its limits. Protecting the people who protect us is essential to the wellbeing of patients and staff alike. Among the many steps that can be taken, the most direct path forward is creating safer, more supportive care environments to support nurse wellbeing.
The American Nurses Association (ANA) is leading that charge, advocating for mental health resources, workforce sustainability, and the recognition nurses have long deserved. This Nurses Week, join the movement: download the ANA Nurses Week social toolkit to celebrate and honor the nurses who show up for all of us, every single day.
Technology That Supports Nurses — Not Adds to Their Burden
One way to create safer and more supportive environments for nurses is through virtual care, which plays a key role in reducing cognitive load and administrative tasks, improving staffing flexibility, and creating safer, calmer environments that support mental wellbeing. Improving nurse satisfaction and retention is the #1 reason health systems implement virtual nursing.
Virtual nursing is reshaping how care teams work, both at the bedside and beyond. Through virtual platforms, nurses and care managers can support bedside teams in real time, helping to educate patients, streamline admissions and discharge paperwork, and automate documentation. This direct, uninterrupted access to patients reduces errors and gaps in the medical record, while freeing floor nurses to focus on what matters most: hands-on patient care. The result is a smarter, more intentional care model — one where RNs, CNAs, and virtual nurses each contribute based on their unique skills and experience, ensuring every patient interaction is handled by the right person at the right time. Beyond the bedside, virtual nursing tools also bridge the gap between hospital staff and external care providers, enabling real-time collaboration that streamlines care transitions and prevents delays in securing post-discharge services.
Caring Out Loud: A Chief Clinical Officer’s Vision for Supporting Nurses
AvaSure’s Chief Clinical Officer, Lisbeth Votruba, MSN, RN, FAONL, CAVRN, joined This Week Health’s Nurses Week podcast to talk about what nursing needs most right now and how technology makes it possible.
A trained nurse practitioner and third generation nurse whose entrepreneurial spirit led her to AvaSure 14 years ago, Lisbeth champions the idea of getting back to old-fashioned, hands-on nursing care and sees ambient listening as one of the most direct paths to get there. Ambient listening is an AI-driven tool that works quietly in the background and can act as a workplace safety tool. If a nurse is feeling in danger, they can simply speak a wake word to trigger an alarm and get help.
Additionally, ambient listening allows nurses to go hands-free while documenting and give their full attention to the patient — no big computer monitor in the way. Lisbeth introduced this concept as “caring out loud”: verbalizing documentation in real time to keep patients connected to their care while shining a light on everything nurses do. It is important to note that when it comes to documentation, nursing workflows can be more complex than physician workflows as they have less of a natural narrative structure. This is why Lisbeth emphasizes that this technology must be built around the nurse so that they do not have to change the way they interact with patients in order for the AI to document the correct takeaways:
“We want to make sure that the tools are trained to serve the nurses, not the nurses having to be trained to serve the tool.”
– Lisbeth Votruba, MSN, RN, FAONL, CAVRN, Chief Clinical Officer at AvaSure
As Chief Clinical Officer at AvaSure, Lisbeth ensures nurses have a seat at the table, bringing the clinical lens necessary to redefine workflows and shape the future of care delivery.
Virtual Care’s Real-World Effect on Nurses
Virtual Care has been supporting nurses across the US, and there are results to prove it. Through scaling their virtual nursing program, Hackensack Meridian Health (HMH) saw outstanding results that directly benefitted their RNs:
- 26% reduction in RN overtime
- 65% reduction in RN traveler hours
- 9% decrease in documentation time for bedside staff
- 12% reduction in length of stay
As their virtual care journey continues, HMH continues to create an improved environment for nurses, and saw a 28% decrease in RN turnover in the first seven months of their recent care units to go live with virtual nursing.
Results like these prove how virtual care eases the workload on nurses, creating a healthier work environment for clinical staff, a better experience for patients, and a more efficient health system overall.
Empowering the Next Generation of Nurses
Virtual nursing isn’t just transforming how we care for patients today; it’s helping to build the nursing workforce of tomorrow. New nurses entering the workforce are already under strain. Virtual nurses serve as an always-available resource for recent graduates and novice nurses — offering real-time mentorship, immediate feedback, and helping new clinicians grow. As virtual care becomes more integrated into hospital workflows and standard care delivery models, it is essential to prepare the next generation of nurses to thrive in this environment. This can include embedding virtual care training into new nurse onboarding and strengthening collaboration between academia and healthcare organizations to support smoother transitions from education to practice.
How AvaSure Cares for Nurses
Nurses are the backbone of healthcare, and for over 18 years, AvaSure has provided them with tools to protect, support, and empower their work. Our intelligent virtual care platform enables virtual care in a diverse range of settings and use cases, with advanced AI, flexible devices, a vast partner ecosystem, real-time insights, and world-class service and support team to guide you every step of your virtual care journey.
AvaSure is committed to clinical partnership, not just technology delivery. Our clinical team is built by nurses, for nurses — and that foundation shapes everything from how the platform is designed to how it is deployed and supported. Our Clinical Implementation team is 100% nurses who maintain active RN licenses, and along with Chief Clinical Officer Lisbeth Votruba, MSN, RN, FAONL, CAVRN, and AvaSure’s Chief Nursing Executive Advisory Board, they lead the clinical vision behind AvaSure. Because AvaSure’s clinical experts have lived the realities of nursing, they are uniquely positioned to design virtual care solutions that reduce burnout rather than add to it. The result is a platform that nurses can embrace and trust.
How to Support Nurses Every Day
National Nurses Week is once a year, but nurses deserve recognition every day. There is nothing more important than protecting those that care for us and consistently showing them our appreciation. AvaSure knows that building safer, healthier environments for nurses is an ongoing collaborative effort, and we are dedicated to making that commitment. From innovative monitoring solutions that reduce the physical and emotional burden on nursing staff, to fostering a culture where nurses feel seen, supported, and valued, AvaSure stands alongside the nursing community not just during National Nurses Week, but through every long shift, every difficult moment, and every triumph in between.
Contact us to see how AvaSure can start supporting your nursing team today.
Common Questions
Virtual nursing is the use of virtual care and advanced AI to assist bedside nurses and hospital staff by automating daily clinical workflows like administrative tasks, intake, rounding, admission & discharge, and more. The American Nursing Association describes virtual nursing as a resource that “support(s) the team at the bedside to alleviate the workload and provide greater satisfaction for both the patients and the nursing staff.”
Nurse burnouts are caused by a number of factors, mainly including chronic understaffing, time-consuming administrative tasks, heavy workloads, workplace violence, long hours, and emotional fatigue. Burnout affects up to 56% of the nursing workforce.
Creating safer and more supportive environments and listening to nurses’ needs is one of the best ways to prevent nurse burnout. Virtual care helps to prevent nurse burnout by reducing cognitive load and administrative tasks, improving staffing flexibility, and creating safer, calmer environments that support mental wellbeing.
Through virtual nursing, nurses and care managers can support teams at the bedside to educate patients, complete admissions and discharge paperwork, automate documentation, and mentor more novice nurses. This allows virtual nurses to have direct, uninterrupted time with patients, leading to less errors or gaps in documentation and freeing up floor nurses to care for their patients at the bedside. This also ensures smoother transitions and shorter delays of care for patients.
Virtual nursing helps with staffing shortages because it allows nurses to return to the bedside and focus on direct patient care, which reduces burnout, increases efficiency in managing workloads, and helps patients receive care more quickly.
Virtual care tools can reduce workload, improve communication, and enhance patient monitoring—helping nurses focus on high-value care while minimizing stress and burnout.
Organizations can invest in supportive technologies, prioritize safe staffing levels, provide mental health resources, and create environments where nurses feel heard and supported.
National Nurses Week, observed each year from May 6–12, recognizes the vital contributions of nurses across the country. It’s also an important moment to spotlight the challenges they face and the need for meaningful support.