
Key Takeaways:
- The Rural Health Transformation Program (RHTP) provides $50B in CMS funding (2026–2030) to strengthen rural hospitals.
- States submitted transformation plans prioritizing technology, workforce resilience, and AI.
- Virtual nursing, TeleHealth, and tele-specialty consults directly align with RHTP goals.
- Hospitals can use RHTP funds to reduce falls, overtime, sitter costs, and specialty care gaps.
- Sustainable virtual care models reinvest efficiency savings beyond federal funding.
What is the Rural Health Transformation Program (RHTP)?
Rural and community hospitals face critical workforce shortages and financial distress, with nearly half operating at a loss as of 2023, according to an AHA analysis of RAND Hospital Cost data. To address these pressures and improve care quality, Congress established the Rural Health Transformation Program (RHTP) under the 2025 One Big Beautiful Bill Act (OBBBA). This $50 billion Centers for Medicare & Medicaid Services (CMS) initiative (FY 2026–2030) provides $10 billion annually to strengthen rural healthcare and offset projected funding gaps.
How CMS Administers RHTP Funding
States are the direct recipients and had to submit a Rural Health Transformation Plan for CMS approval. Half of the funding is divided equally among participating states—guaranteeing at least $100 million per year for five years if all states join—while the other half is distributed via a CMS formula. This massive pool supports infrastructure, technology, and workforce improvements for nearly 1,800 rural hospitals and 60 million residents.
How Critical Access Hospitals (CAHs) Benefit from RHTP Funding
While all rural providers are eligible, the nation’s 1,350 Critical Access Hospitals (CAHs) stand to benefit most, particularly in the Midwest and states like Texas, Iowa, and Kansas. By investing in these hospitals, the RHTP aims to prevent closures, preserve essential services like emergency and maternity care, and improve health outcomes in rural America.
Contact AvaSure to discuss how you can use RHTP funding for virtual care.
How can telehealth and virtual care benefit rural hospitals?
RHTP applications from numerous states have revealed a priority among rural hospitals: the use of telehealth and virtual care to help extend and improve care where things like specialty care are often unavailable.
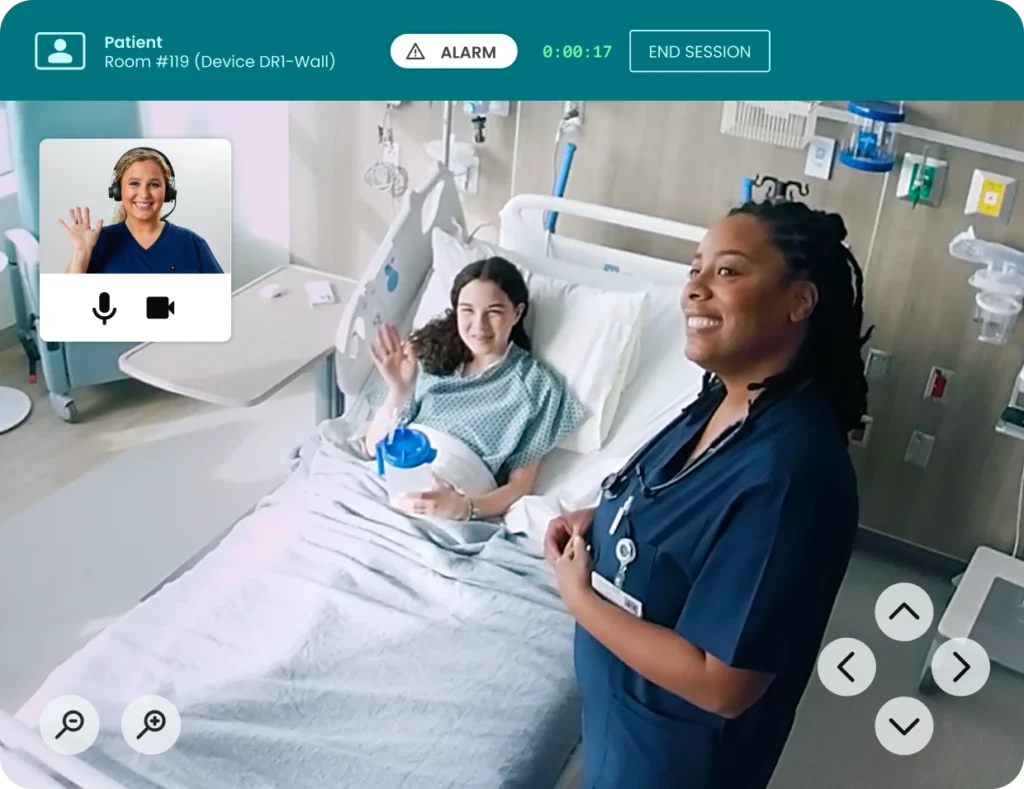
By integrating telehealth, rural facilities can bridge the “specialty gap,” allowing local doctors to consult with world-class neurologists or cardiologists in real-time without transferring the patient. This “keep it local” approach not only improves patient outcomes during emergencies but also stabilizes the hospital’s finances by retaining admissions and reducing the reliance on expensive traveling staff. In addition, by leveraging AI and virtual care, rural hospitals can expand local access and boost financial sustainability while delivering higher-quality care. These innovations do more than just improve patient outcomes and ROI; they actively reduce safety risks like falls, alleviate staff burnout, and foster collaborative models of care. See how Hackensack Meridian Health improved nurse satisfaction and patient outcomes through virtual nursing.
How do states plan to use their funding for the Rural Health Transformation Program (RHTP)?
States submitted plans in December 2025 that had to meet specific criteria defined by CMS. Funding for these plans was released in January 2026. The plans had to address how hospitals will:
- Prioritize the use of new and emerging technologies including AI to improve rural health outcomes
- Improve access to care locally
- Enhance quality metrics for rural patients
- Foster partnerships (e.g. small hospitals collaborating with larger systems) and ensure financial stability of rural providers
- Tackle causes of rural hospital closure
How can hospitals leverage RHTP funding?
1. Engage State RHTP Leadership
Coordinate with your state health department or Medicaid agency to include virtual care in your Rural Health Transformation Plan. Highlight its impact on workforce resilience and patient safety.
2. Develop a Turnkey Proposal with AvaSure
Work with AvaSure to submit a fundable plan covering:
- Platform deployment and configuration
- Clinical and operational workflow redesign
- Staff training and ongoing support
- Continuous performance measurement
3. Measure and Report Outcomes
To strengthen your case, align the stated goals to the RHTP program and track them. The outcomes that AvaSure has benchmarked with partner hospitals with virtual care programs are:
- 72% improvement in 1:1 sitter usage
- 11.6% improvement in length of stay
- 26% improvement in RN overtime
- 30-50% improvement in falls
4. Build a Sustainable Model
Reinvest efficiency savings and improved performance outcomes to sustain virtual nursing operations post-RHTP funding.
AvaSure’s maturity model provides a strategic roadmap for health systems to transition from initial pilots to a fully integrated virtual care delivery system. It serves as a vital framework for leaders to benchmark their current capabilities and identify the specific infrastructure and workflow milestones required to reinvest efficiency savings and sustain high-performance virtual nursing long after the conclusion of RHTP funding.

How AvaSure Aligns with the Rural Health Transformation Program
AvaSure, the industry leader in virtual nursing and continuous patient monitoring, helps hospitals extend nursing capacity, reduce falls and sitter costs, and enhance care quality through a proven operational model. AvaSure’s virtual care platform is fully aligned with RHTP’s focus on technology-enabled workforce transformation.
RHTP Funding Categories Supported by AvaSure:
- Workforce development and modernization
- Technology-enabled patient care and safety
- Training and technical assistance
- Quality and efficiency improvement initiatives
The Rural Health Transformation Program prioritizes initiatives that stabilize and modernize the healthcare workforce, improve patient safety, and enable sustainable operations in rural hospitals. AvaSure supports all three objectives by bringing virtual nursing and continuous observation into daily hospital operations:
- Virtual Nursing: Augments bedside teams with remote nurses who handle admissions, discharges, and patient education to reduce admin burden.
- Continuous Observation (TeleSitting): Centralized video observation reduces falls, elopements, and 1:1 sitter costs.
- Specialty Consults: Consult with specialists in another location to expand care without having to move your patient.
This in turn leads to benefits such as:
- Workforce Flexibility: Reduces overtime, improves staff retention, and increases productivity.
- Patient Safety: Delivers continuous monitoring and rapid response support.
Ultimately, access to care and physician specialists remains one of the most pressing challenges for rural hospitals, leading many to prioritize specialty health and telehealth consults in their strategic applications. To effectively remedy these gaps, it is essential to select a virtual care platform that leverages the specific partnerships necessary to bridge the distance between patients and specialized expertise.
How Can AvaSure Help?
AvaSure’s partnership with Equum Medical, a telehealth-enabled clinical workforce organization, will provide rural hospitals with easy access to virtual specialty consults. The company’s broad portfolio of services addresses the driving challenges of Access and Capacity for health systems, including multi-specialty telemedicine, critical care, virtual nursing, virtual sitter monitoring, and telemetry. Solutions include:
- Inpatient tele-specialty consults (e.g., neurology/stroke, psychiatry, cardiology, nephrology, infectious disease, pulmonology, and more)
- Tele-ICU and critical care support, including surge capacity and after-hours coverage
- Virtual hospitalist support for nights, weekends, and hard-to-staff locations
- Care coordination that helps reduce avoidable transfers, keep patients local, and support patient flow with integrated virtual nursing capabilities across care venues
These solutions strengthen financial sustainability while offering scalable, broadband-friendly technology specifically designed for the unique constraints of rural settings. Unlike typical telehealth partnerships that add separate point solutions, the integrated model runs on a single platform that many hospitals already use for virtual nursing and patient observation, paired with Equum’s physician and clinical programs.
Your RHTP Virtual Care Strategy
AvaSure equips rural hospitals with innovative virtual care and AI-powered solutions that expand local access, enhance care quality, and strengthen financial sustainability. By reducing adverse events like patient falls, easing workforce burdens, and fostering collaborative models of care, AvaSure helps rural providers meet and exceed the goals of the Rural Hospital Transformation Program.


