Earlier this summer I attended a webinar presented by the National Quality Partners Action Team to Prevent Healthcare Workplace Violence. The group includes representatives of healthcare organizations such as Cleveland Clinic Lutheran Hospital and the Department of Veterans Affairs and professional organizations such as the Emergency Nurses Association and the American Nurses Association. The team was convened by the National Quality Forum in October 2019 to increase awareness about the need to improve healthcare worker safety.
The event was edifying and covered a lot of familiar ground, but something was missing: A solution that actually prevents abuse of staff.
The National Institute for Occupational Safety and Health defines workplace violence as physical assault, threatening behaviors and/or verbal abuse towards persons at work or on duty. Healthcare workers are four times more likely to suffer violence than workers in other industries. Evidence shows workplace violence is tremendously under-reported by nurses. Hospital leaders are challenged on how to address the problem.
During the webinar, the presenters addressed the physical and emotional harm, stress, and cost of threats and assaults on health workers. In addition, the panel addressed the many challenges to identifying, tracking, trending and preventing workplace violence. The panelists outlined four recommendations for change: standardizing definitions and data collecting, analyzing and sharing data, investing in safety, and collaborating and scaling efforts. (For more, see the team’s recent issue brief.)
Interventions offered include incident reporting, data collection and greater transparency. However, much research confirms that reporting episodes of violence in the workplace is dependent on nurses’ filing reports to hospital leaderships. Given that nurses believe little will be done to reduce workplace assaults in response to such reports, transparency is unlikely to improve simply by wishing it were better.
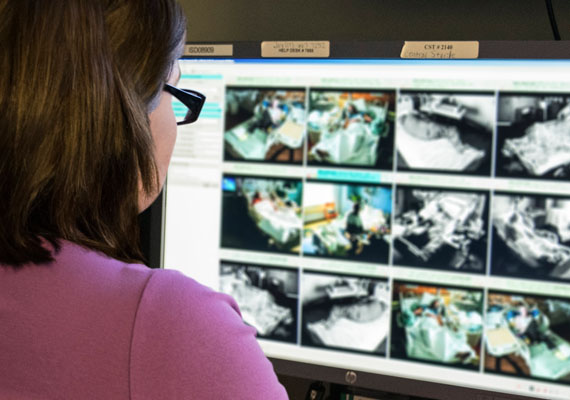
As I listened, I waited (in vain) for this newly formed action team to inform the audience of the proven success of remote safety monitoring in capturing, trending and tracking actual patient assaults on nurses, and the success of monitoring staff in both warning nursing staff about potentially problematic patients and using audio interventions to de-escalate situations that develop.
Technology such as this is not exactly new to healthcare systems. Remote safety monitoring has demonstrated results on patient outcomes for over a decade, and now there is published evidence of its effectiveness in preventing attacks on staff as well as accurately collecting, classifying, tracking and trending reliable data.
I should know, as I co-authored two large-scale national descriptive correlation studies on this issue with Lisbeth Votruba and Jill Kaminski. We used AvaSure’s Online Reporting of Nursing Analytics (ORNA) tool, a cloud-based data program that documents comparative efficacy by a host of different parameters, including by hospital, hospital systems, unit, patient and patient condition.
One of those articles, published last December in American Nurse Today, describes the value of AvaSure in documenting, trending and preventing workplace safety incidents. Reviewing the ORNA database, the article found that over a year, monitor staff reported witnessing 136 incidents of verbal and physical abuse of staff. Another 5,458 events were prevented by the intervention of the monitor technician, 90% of them by verbal intervention alone.
Another study published late in 2019 in the Journal of Nursing Care Quality found that monitor staff intervened to avoid 40 workplace violence events for every one that occurred – a 97% reduction.
After hearing about and reading about violence against nurses for most of my career, this data is music to my ears. I encourage every healthcare leader and health system board member to read those articles and act on them, committing to preventing physical and emotional violence against the people who work for you by investing in proven technology and programs and NOT relying on workforce staff reports or incident reports filed long after events have occurred.
Patricia A. Quigley, PhD, MPH, MS, APRN, is a nurse consultant, AvaSure Advisor and a leading expert on patient falls.